Childbirth is a unique and transformative experience, filled with anticipation, excitement, and, let’s face it, a fair amount of anxiety. One of the most common concerns for expectant mothers revolves around the pain associated with labor and delivery. This is where the concept of an epidural birth comes into play. But what is epidural birth? This article aims to demystify the process, benefits, and potential risks associated with epidural birth, providing you with the knowledge you need to make an informed decision.
What is Epidural Birth?
Epidural birth, as previously mentioned, is a childbirth process where an epidural anesthesia is used to manage the pain of labor and delivery. The term ‘epidural’ refers to the epidural space in the spine where the anesthesia is administered. This form of anesthesia is regional, meaning it targets a specific area of the body – in this case, the lower body.
The Science Behind Epidural Anesthesia
The epidural anesthesia works by blocking the nerve impulses from the lower spinal segments. This results in decreased sensation in the lower half of the body. The medication used in an epidural is typically a combination of a local anesthetic and a narcotic. Local anesthetics like bupivacaine or lidocaine numb the body and block pain, while narcotics such as fentanyl or morphine decrease pain signals being sent to the brain.
The beauty of epidural anesthesia is that it can be adjusted to the individual needs of the mother. The amount of medication can be increased or decreased, and the epidural can be topped up if necessary. This is particularly useful in long labors where pain management over an extended period is required.
The Process of Epidural Administration
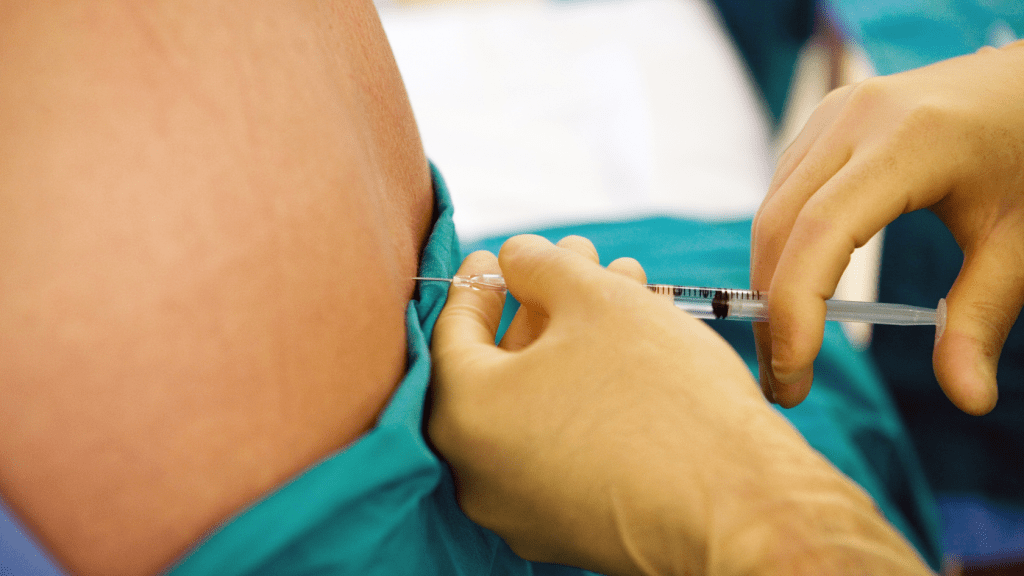
The administration of an epidural involves a series of steps. First, the mother is asked to either sit up or lie on her side, with her back curved outwards. This position allows the anesthesiologist to locate the epidural space in the spine more easily. A local anesthetic is then applied to numb the area where the epidural needle will be inserted.
Once the area is numb, a larger needle is carefully inserted into the epidural space, which is located outside the membrane that protects the spinal cord. A small catheter is threaded through this needle, and the needle itself is removed, leaving the catheter in place. This catheter is used to deliver the epidural medication, which typically begins to take effect within 10 to 20 minutes.
Read about stages of labor.
The Role of the Mother During an Epidural Birth
Despite the numbing effect of the epidural, the mother remains fully conscious and active during labor. She can still feel pressure and movement, which is beneficial when it comes time to push. However, the intensity of these sensations can vary depending on the specific mix of medications used in the epidural.
In some cases, a ‘walking epidural,’ also known as a combined spinal-epidural (CSE), may be used. This technique involves a lower dose of medication, allowing the mother more ability to move her legs and even walk around during labor. This can help the mother feel more in control of her birthing process.
How is Epidural Birth Different from Natural Birth?
Here are some key differences between an epidural birth and natural birth:
Pain Management: The most significant difference between an epidural birth and a natural birth is the approach to pain management. In an epidural birth, medication is used to numb the lower half of the body, significantly reducing the pain of labor and delivery. In a traditional birth, no epidural anesthesia is used. Pain may be managed through other methods such as breathing techniques, movement, water birth, or other non-pharmacological pain relief methods.
Mobility During Labor: With an epidural, the mother’s mobility can be limited once the epidural is in place. While there are “walking epidurals” that allow for more movement, many women will be confined to bed once the epidural is administered. In a traditional birth, women are often encouraged to move around, change positions, walk, or even use a birthing ball to help cope with the pain and assist in the progression of labor.
Use of Medical Equipment: During an epidural birth, continuous fetal monitoring is usually required. This means the mother will have monitors strapped to her abdomen to keep track of the baby’s heart rate. An IV line is also typically placed to administer fluids and medications. In a natural birth, there may be less reliance on medical equipment, and intermittent monitoring of the baby may be possible, depending on the mother’s and baby’s condition.
Potential for Interventions: Epidural births have a slightly higher association with certain interventions, such as the use of Pitocin to speed up labor or the need for a vacuum or forceps during delivery. This is not to say that these interventions will definitely occur, but the likelihood can increase. In a traditional birth, assuming no complications arise, there’s often less medical intervention.
Recovery: Recovery can vary greatly from woman to woman and birth to birth. However, women who have had an epidural may experience some side effects such as back soreness at the site of the epidural, headaches, or a temporary decrease in bladder control. Women who have a traditional birth may experience more perineal soreness or pain, particularly if they’ve had a tear, but avoid the potential epidural-related side effects.
Learn more here about natural birth.
It’s important to note that every woman’s experience with labor and delivery is unique, and there’s no one-size-fits-all approach. What’s most important is that the birthing process is safe for both mother and baby, and aligns as closely as possible with the mother’s personal preferences and comfort level.
Preparation for an Epidural Birth

Preparing for an epidural birth involves both physical and mental preparation. Here are some steps expectant mothers can take to prepare for an epidural birth:
Education: Understanding the process of an epidural, its benefits, and potential risks is crucial. Attend childbirth classes, read books, watch educational videos, and use reliable online resources to educate yourself about the process. Knowledge is power, and the more you know, the better prepared you’ll be.
Discuss with Your Healthcare Provider: Have a conversation with your obstetrician or midwife or anyone from your healthcare provider about your desire to have an epidural. They can provide you with specific information tailored to your health history and the policies of the hospital or birthing center where you plan to deliver.
Create a Birth Plan: While it’s important to understand that birth plans may need to change based on circumstances, having a plan can help you feel more prepared. Include your wish for an epidural in your birth plan, and discuss this plan with your healthcare provider.
Understand the Timing: An epidural is typically given once active labor has started and the cervix is about 4 to 5 centimeters dilated. However, the timing can vary based on different factors. Discuss the timing with your healthcare provider so you know what to expect.
Prepare Physically: Epidurals are administered in the lower back. Therefore, maintaining a healthy weight and staying active during pregnancy can help make the administration of the epidural easier. Regular exercise, such as prenatal yoga or walking, can help keep your back strong and flexible.
Mental Preparation: The thought of childbirth can be daunting, and the idea of having a needle inserted into your back might add to that anxiety. Mental preparation is key. Practice relaxation techniques, such as deep breathing, visualization, or meditation, to help manage anxiety and promote a positive mindset.
Plan for Post-Birth: After an epidural, it may take some time for the medication to wear off, and you might experience some temporary numbness in the lower half of your body. Arrange for help in the hours following birth, as moving around may be challenging initially.
Remember, every birth is unique, and what works best will depend on your individual circumstances and preferences. Always consult with your healthcare provider when making decisions about your birth plan.





